If there’s one concern that every woman should have it’s about maintaining healthy bones. If you live long enough, you will likely experience significant bone loss. Just as you lose muscle mass with age, you lose bone as well. As bone density declines, the risk of breaking a bone with minimal trauma goes up. People with osteoporosis can even develop spontaneous bone fractures – a bone snaps with only minimal trauma. Sometimes, something as minor as a coughing spell can fracture a bone weakened by osteoporosis.
Osteoporosis can also distort your body’s alignment. You’ve probably seen women who have the so-called dowager’s hump, a condition where the front portions of the thoracic vertebrae collapse and the upper spine curves forward. These people are forced into a position where the head always points downward because their bones are ravaged by osteoporosis.
How Osteoporosis Comes About
How does osteoporosis start? You begin to lose bone after the age of 30 and the loss speeds up after menopause. In fact, women lose up to 2% of their bone density each decade after menopause. It’s a gradual but relentless process. Hopefully, you built up enough bone early in life that this loss still leaves you with enough healthy bone to avoid fractures. However, it’s important to monitor your bone density to make sure you don’t have osteopenia or true osteoporosis. Osteopenia is where bone density is lower than it should be but not enough to be classified as osteoporosis.
The gold standard for determining bone density is the DXA scan, also called dual-energy X-ray absorptiometry). This test measures bone density in the hips and lumbar spine. Based on the results, the technician generates a T-score based on bone density. A T-score tells you how dense your bones are relative to a healthy 30-year-old. If a T-score is 25% lower than the average, healthy 30-year-old, it’s classified as osteoporosis. DXA scans have their drawbacks. For example, they expose you to a small amount of radiation and you have to go to a special center to get your bone density tested. However, a DXA scan only exposes you to very low-dose radiation, about a tenth of what you get from a chest x-ray.
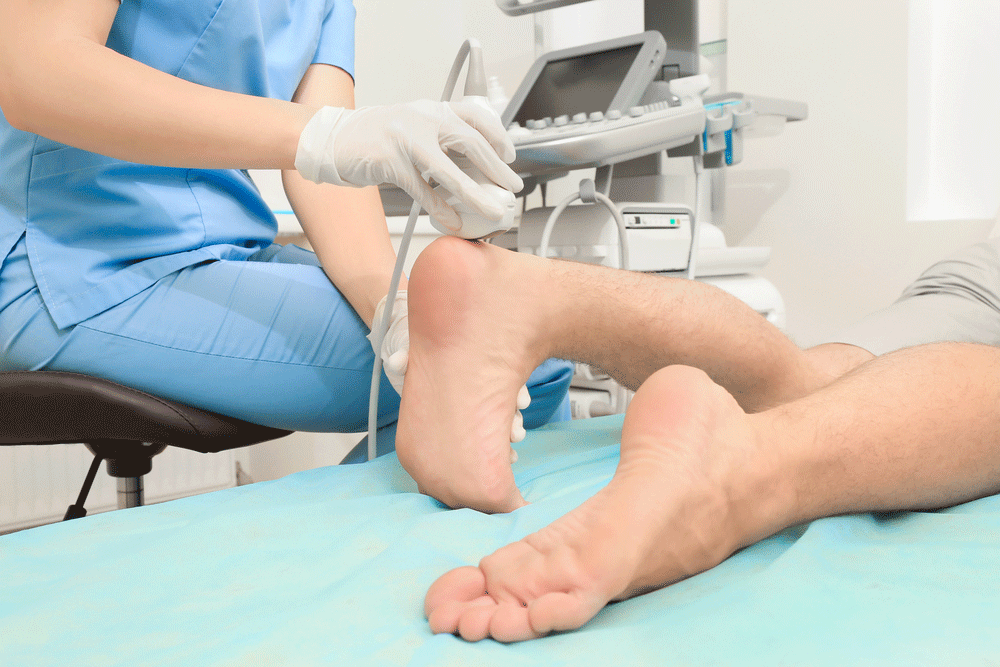
For convenience, many community-based wellness centers use an alternative method to measure bone density, an ultrasound scan of the heel. This test is simple, easy to do, uses portable equipment, and doesn’t expose you to radiation. But, is are heel scans a good alternative to the more advanced DXA scan for measuring bone density?
How Accurate Are Heel Scans?
Heel scans certainly have their advantages, but you ultimately want a screening tool to be accurate. Heel scans shoot sound waves through the heel to measure bone density. Sound waves behave differently when bones are dense as opposed to when bone density is low. Heel scans can give you a rough idea of how dense your bones are, but you’re only measuring one part of your skeleton, your heel. A DXA scan measures hip and spine density as well. That’s important since bone density can vary at different sites. Someone can have a low bone density in the hip and have a normal bone density in the spine. A DXA scan can tell you what your bone density is at various locations. A heel scan cannot.
Where the heel scan is helpful is in determining whether you need further testing, in other words, a DXA scan. If the heel scan is abnormal, it raises a red flag and suggests that you need further testing. Heel scans, unlike a DXA, also can’t follow changes in bone density over time. So, a heel scan isn’t ideal, as you’re getting limited information and only at the heel.
Another advantage of a DXA scan is some hospitals can perform another type of scan at the same time. This scan , called a vertebral fracture assessment (VFA) analyzes the shape and height of your bones and looks for discrepancies that might suggest a compression fracture, a type of fracture in the spine that’s often silent. This additional test is particularly helpful if you have a strong family history of osteoporosis or are at high risk for other reasons. Risk factors for osteoporosis include:
- Being female
- Being over the age of 50
- Being Caucasian or Asian
- A family history of osteoporosis
- Menopause, either natural or surgical
- Being underweight or small-boned
- A history of a bone fracture
- Being sedentary
- Smoking
- Excessive use of alcohol
- Taking certain medications that increase bone loss, such as steroids
- History of an eating disorder, like anorexia nervosa or bulimia
So, it’s easy to see why osteoporosis is so common. Many people have one or more of these risk factors. If you don’t have risk factors, experts recommend that you get a DXA scan by age 65. Will a heel scan suffice? Heel Scans won’t give you your T-score because you can’t calculate a T-sore from a single site. By the time you reach 65, you should know your T-score and that’s one of the biggest limitations of a heel scan. If you’re under the age of 65, a heel scan is acceptable, but it only looks at bone density at a single site. So, don’t rely on it too much to tell you the status of your bones.
If you’re at high risk of osteoporosis, you may need screening before age 65. Talk to your physician about your risk factors and get their advice on when to get your first bone density screening.
The Bottom Line
Heel scans are widely available but don’t depend on them to reliably tell you whether you have osteoporosis. Once you reach the age of 65, or earlier if you’re at high risk, get a DXA scan so you can get a reliable T-score you can follow over time. Just as importantly, lead a bone-healthy lifestyle by optimizing your nutrition and doing high-impact exercise and resistance training to help preserve your bones as you age.
References:
- University of California, Berkeley Wellness Letter. October 2017.
- Orthop Rev (Pavia). 2016 Jun 27; 8(2): 6357.
- National Osteoporosis Society. “Bone Density Scanning and Osteoporosis”
- National Osteoporosis Foundation. “Are You at Risk?”
Related Articles By Cathe:
5 Nutrients Other Than Calcium You Need for Healthy Bones
Can Walking Lower Your Risk of Osteoporosis?
The 3 Best Types of Exercise for Bone Density and Health
Is Eating Too Much Sugar Harmful to Your Bones?
If You Have Strong Muscles, Are You More Likely to Have Strong Bones?
How the Female Spine Changes with Age and Why It Matters
Are Certain Types of Exercise Bad for Bone Health?
Does Yoga Improve Bone Health?
How Effective Is Step Training for Improving Bone Density?
Vitamin K2: The Key to Keeping Your Bones Strong and Arteries Clean?