One of the most common health problems in men and women over 50 is osteoarthritis, although they’re not always aware of it. If you looked at x-rays from people in this age group, you would likely see the telltale signs of this degenerative condition in the knees, hips, hands, or other joints. That doesn’t mean that everyone with x-ray evidence of osteoarthritis has significant joint pain or stiffness. Some people only have evidence on imaging studies and are spared the pain and stiffness the disease can cause, at least for a while.
In fact, the symptoms can be silent sometimes for years or even a lifetime. Still, arthritis of all types is the most common cause of disability in the United States. Joint replacement surgery, replacing arthritis hips and knees, is now a commonplace surgery – but it’s not a gamechanger for everyone. Plus, the recovery period from surgery is six weeks or longer. That’s why it’s best to prevent or at least slow the onset and progression of osteoarthritis.
At one time, doctors told patients to avoid high-impact exercise if they had osteoarthritis. We now know that moderate physical activity may improve the symptoms of various forms of arthritis, including osteoarthritis. But what about diet? Is there any evidence that the type of diet you eat impacts the progression of osteoarthritis?
Diet and Osteoarthritis
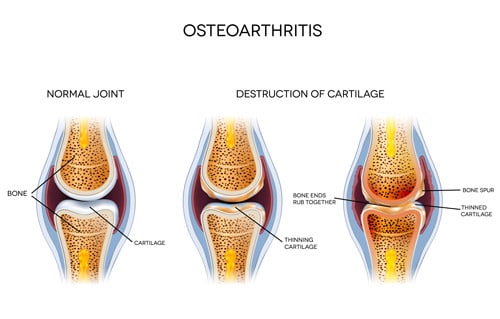
Osteoarthritis is called a degenerative disease. It’s caused by damage to the cartilage that covers the ends of bones within a joint. Cartilage has the important function of preventing friction with movement. Yet, experts now believe that it’s also an inflammatory disease. What happens is joints get damaged initially by “wear and tear.” Once a joint becomes damaged, immune cells go into overdrive to repair the damage. As you might expect, inflammation makes the pain and stiffness worse.
How do we know there’s an inflammatory component? Researchers discovered that there are markers of inflammation in the synovial fluid, the fluid that surrounds the cartilage inside the joint, in people with osteoarthritis. Based on this, you might ask whether an anti-inflammatory diet would slow the progression of osteoarthritis or at least ease the symptoms.
There is evidence that some foods can worsen inflammation while others have a modest anti-inflammatory effect. On the plus side, omega-3s in fatty fish, nuts, fruits, vegetables, and some spices, including turmeric, ginger, and cinnamon help ease inflammation. At the other end of the spectrum, processed foods and foods high in omega-6s, like red meat and processed vegetable oils fuel inflammation. So, eating more whole foods, particularly plant-based foods, may improve the symptoms of arthritis by reducing inflammation. Whether an anti-inflammatory diet slows progression is still unknown.
Could a High-Fiber Diet Prevent Osteoarthritis?
If there’s one dietary component that Americans fall short of it’s dietary fiber. You find fiber naturally only in plant-based foods – whole grains, legumes, nuts, fruits, and vegetables. If you eat a very low-carb diet or build your diet around processed foods, you’re probably won’t get enough fiber in your diet. What does this have to do with osteoarthritis? A new study published in Family Practice News showed that a diet higher in fiber was linked with a lower risk of developing symptomatic osteoarthritis. To reach this conclusion, researchers followed 4,796 middle-aged and older men and women for 4 to 8 years. They used a food frequency questionnaire to determine how much dietary fiber they ate on a daily basis and compared it to knee x-rays.
What they found was participants who consumed at least 25 grams of dietary fiber daily were at lower risk of developing osteoarthritis. In those already having the condition, the fiber was linked with a reduced incidence of moderate or severe knee pain. So, a high-fiber diet may improve the symptoms as well. The results held even when the researchers adjusted for a long list of other factors that could have influenced the results.
Although you can’t say based on this study that dietary fiber and osteoarthritis are causally linked, it does bear further exploration. Even without being able to say a high-fiber diet prevents osteoarthritis, you can’t go wrong adding more fiber to your breakfast, lunch, and dinner plates. Don’t forget a diet high in fiber is also linked with a lower risk of heart disease. Plus, it increases satiety and helps with weight and blood sugar control.
What Else Can You Do to Keep Your Joints Healthy?
One risk factor for osteoarthritis you have little control over and that’s aging. Since osteoarthritis is a disease of wear and tear, the longer you live, the likelier you are to get it. Genetics are a factor too. Osteoarthritis tends to run in families and you can’t choose who your parents are. One factor you have more control over is body weight. People who are overweight or obese place more pressure on their joints and this leads to greater cartilage breakdown. Regular physical activity helps with weight control while weight training strengthens the muscles that support the joints. Use good form when you lift weight since injuries around a joint place you at greater risk of osteoarthritis.
The Bottom Line
There isn’t a surefire way to prevent osteoarthritis, although you may lower your risk by maintaining healthy body weight, exercising, and eating a whole food diet that’s high in fiber. Of course, a diet like this may reduce your risk of developing a variety of health problems and help with weight control as well. A healthy diet and lifestyle is the key to staying healthy and functional as you age – and the best time to start is now. Exercise and a healthy, high-fiber diet consisting of anti-inflammatory foods may help tame the symptoms and, possibly, even slow its progression.
References:
Family Practice News. “Fiber May Play Role in Lessening Knee Pain, OA Development” December 2016.
WebMD. “Inflammation May Affect Osteoarthritis”
Harvard Health Publications. “New ways to beat osteoarthritis pain”
Harvard Health Publications. “Eat more fiber-rich foods to foster heart health”
Harvard T.H. Chan School of Public Health. “Fiber”
Arthritis Foundation. “Osteoarthritis Prevention: What You Can Do”
Related Articles By Cathe:
Are the Joint Aches You’re Experiencing Due to Arthritis?
Can Regular Exercise Prevent Osteoarthritis?
How Your Joints Age & What You Can Do to Slow It Down

